Increasing patient numbers, clinician burnout, rising costs of operation, and rising chronic diseases are pushing hospitals to their limits. Simultaneously, huge volumes of medical information are not fully used, which suppresses diagnosis and restricts preventive care.
The point of concern is that conventional healthcare models are unable to sustain such a rate of demand. Efficiencies in administration, workforce deficiencies, and delayed treatments are increasing.
However, artificial Intelligence can serve as a viable way out. AI is changing the way healthcare is delivered with predictive diagnostics and customized treatment plans, automated documentation, and real-time patient monitoring.
In fact, the global AI in healthcare market was valued at roughly $39.3 billion in 2025 and is expected to surpass $1 trillion by 2034. It will not be replacing doctors in the future, but giving them smarter, faster, and more scalable systems.
Key Takeaways
- The Problem: The healthcare systems experience growing patient demands, workforce deficits, ineffective data organization, elevated operational expenses, and a growing burden of pressure to perform better without compromising compliance and patient confidence.
- The Solution: Artificial Intelligence healthcare allows predictive diagnostics, automation of the workflow, real-time information, individual treatment regimen, and better clinical decision support, which improves efficiency and the quality of patient care.
- How SoluLab Helps: SoluLab develops AI native development platform, scalable AI healthcare infrastructure, including intelligent diagnostics software and data analytics software, AI-powered applications, and interoperable systems designed to enhance operations and deliver quantifiable healthcare results.
Current State of AI in Healthcare
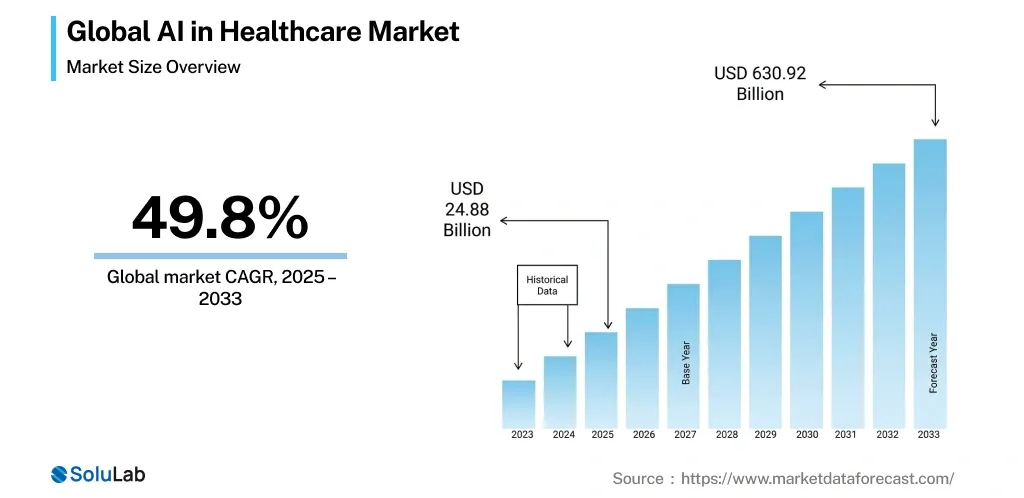
Artificial intelligence is no longer experimental in healthcare. It is also working towards diagnostics, drug research, hospital operations, and patient engagement, reinventing care delivery globally. The global AI in healthcare market is expected to reach 630.92 billion by 2033.
- Artificial intelligence in Diagnostics: Computer algorithms can now help radiologists locate cancers, fractures, and neurological conditions more quickly and with higher precision. Recent articles in Nature Medicine demonstrate that AI systems perform on par with, or even outperform, specialists in detecting breast cancer, thereby improving the overall rate of early cancer diagnosis.
- AI-Powered Drug Discovery: AI reduces drug discovery timelines by analyzing large biological datasets and screening potential compounds. According to McKinsey, AI has the potential to reduce the time needed to discover new drugs in the early stages by up to 40 percent and enable the pharmaceutical industry to lower the cost of R&D and shorten clinical trial durations.
- Clinical Decision Support Systems: Clinical decision support tools are AI-based technologies that analyze a patient’s medical history, labs, and medical literature to help physicians during treatment planning. Deloitte states that hospitals with developed analytics and AI-driven systems of decision-making can document improvements in the quality of care and operational efficiency.
- Virtual Health Assistants and AI Chatbots: Chatbots are used in healthcare and can help patients book appointments, identify symptoms, and answer questions 24/7. Juniper Research posits that healthcare chatbots can save the sector millions of dollars annually by reducing administrative staff and improving patient response times.
- Automation of Hospital Workflows: Hospital billing, documentation, scheduling, and supply chain management are automated using AI. Accenture research suggests that the US healthcare economy could save up to 150 billion US dollars annually through AI-based workflow automation, reducing operational waste.

Key Drivers Accelerating AI Adoption in Healthcare
The global healthcare sector is quickly embracing artificial intelligence as financial constraints, data explosion, patient demands, and the emergence of digital care frameworks reform the way healthcare facilities deliver efficient, patient-centered, and scalable healthcare services.
- Increasing Healthcare Costs: Global healthcare expenditure amounted to about 9.8 trillion, just under 10 percent of global GDP. Automation, predictive analytics, and workflow optimization are among the ways AI can lower administrative expenses, which account for up to 2530 percent of hospital expenses.
- Expansion of Healthcare Data: Healthcare produces some 30 percent of all data on the planet and is increasing by 36 percent per year. AI can help providers work effectively with medical imaging, electronic health records, and genomic data, transforming complex data into actionable clinical insights.
- Need for Personalized Medicine: Precision medicine is booming at a very high rate, and the market is expected to reach over 175 billion across the world by 2030. AI examines genetic, lifestyle, and clinical data to prescribe individualized treatment to improve outcomes and minimize unnecessary interventions.
- Growth of Telemedicine: The use of Telehealth had reached approximately 38 times that recorded before the pandemic. AI can improve the accessibility of virtual consultations through symptom triage, automated documentation, and real-time monitoring, reducing providers’ workload.
Why Healthcare Organizations Partner with AI Development Companies
Healthcare organizations partner with AI development companies to overcome technical complexity, accelerate innovation, and deploy scalable, compliant solutions that improve patient outcomes while reducing operational costs and inefficiencies.
- Access to Specialized AI Expertise: AI development companies bring deep expertise in machine learning, data engineering, and healthcare compliance, enabling organizations to build accurate, reliable, and production-ready AI solutions without hiring large in-house teams.
- Faster Time-to-Market: With proven frameworks, tools, and pre-built models, AI partners accelerate development cycles, helping healthcare providers deploy solutions quickly and start realizing value without long implementation delays.
- Integration with Existing Systems: AI development companies ensure smooth integration with EHR systems, hospital software, and legacy infrastructure, minimizing disruption while enhancing workflows and maintaining data consistency across platforms.
- Regulatory Compliance and Security: Experienced AI vendors understand healthcare regulations like HIPAA and GDPR, ensuring secure data handling, audit trails, and compliance-ready systems that reduce legal risks and protect patient information.
- Cost Optimization and Scalability: Partnering with AI companies helps reduce development and operational costs by leveraging scalable cloud infrastructure, reusable components, and optimized architectures designed for long-term performance and growth.
Read Also: How Healthcare Startups in the USA Leverage Generative AI to Cut 40% Costs?
Real-World Use Cases of AI in Healthcare
Artificial intelligence is moving beyond pilot projects to the mainstream of the healthcare infrastructure and is providing quantifiable benefits to diagnoses, treatment planning, and patient outcomes in a variety of medical specialties.
1. AI in Oncology
Artificial intelligence models are assisting in the earlier detection of cancers and precision in the treatment. In research published in Nature, AI systems were as capable as radiologists in detecting breast cancer, and it lowers false positives and negatives, as well as assisting in quicker, data-driven decision-making in oncology.
2. AI in Cardiology
AI-based imaging and ECG analysis can be used in cardiovascular care to enhance the timely identification of heart conditions. Research mentioned in The Lancet found that machine learning-based methods detected cardiac abnormalities with an accuracy rate of more than 85 percent, which helped to implement faster intervention and minimize the risk of mortality.
3. AI in Radiology
The radiologists are now assisted by AI agents in healthcare that identify anomalies in X-rays, CT scans, and MRIs. In a study published by Radiology, it has been found that AI systems are capable of saving up to 30 percent of time on image interpretation and have high diagnostic accuracy.
4. AI in Mental Health
The AI-based tools process the speech pattern, behavior, and online activity to detect the signs of depression, anxiety and AI in drug discovery at early stages. AI has the potential to increase access to mental health screening among underserved groups, as studies cited by the World Health Organization indicate.
What Are the 2026 Future Trends of AI in Healthcare?
In 2026, AI healthcare solutions will be in a decisive stage and no longer pilot experiments but a visible impact, increased governance, scalability, and actual clinical collaboration between humans and intelligent technologies.
1. ROI Proof Over Promise
The healthcare leaders are no longer seeking hype, but results. Grand View Research estimates the global AI healthcare market to reach more than $180 billion by 2030, and grow by more than 35 percent each year. Hospitals are focusing on cutting costs, accelerating diagnostics, and efficiency of operations, and will increase AI budgets only afterward.
2. Organizational Readiness
It has been providing AI-ready infrastructure, data modernization, and migration to the cloud. According to McKinsey, more than 60 percent of healthcare executives intend to invest more in AI in the next three years, with the areas of concern being integration, workforce training, and interoperability.
3. Artificial Intelligence-Human Cooperation Is Forming.
Generative AI in US Healthcare startups is reinforcing a critical shift—AI is enhancing clinicians, not replacing them. Research published in The Lancet Digital Health shows AI-supported radiology can improve diagnostic accuracy by up to 20 percent. Administrative burdens are reduced, while clinicians retain control through intelligent decision-support tools.
4. The Staging of AI Agents is Progressively Necessary
The direction of healthcare organisations is towards multi-agent AI systems, which organize the diagnostics, scheduling, documentation, and monitoring of the patient. Gartner estimates that more than half of large businesses will have implemented AI orchestration platforms by the year 2026 to operate complex business processes.
5. The Tech with AI Governance
As the regulation increases, the governance structures become harder. The World Health Organization has also given directives on how AI is used ethically in the medical field, whereas regulatory authorities are enhancing the privacy requirements. Audit trails and transparent algorithms are becoming compulsory.
Read Also: AI Healthcare in the UAE
How SoluLab Helps Companies Build AI in Healthcare Solutions?
SoluLab is an AI-native company that leverages AI within its own workflows to deliver healthcare solutions faster, reduce development costs, and help organizations build scalable, efficient, and compliant AI systems.
With AI driven development approach, here are the AI in healthcare services we provide:
- AI Healthcare Platform Development
- Healthcare Data Analytics & Predictive Modeling
- Generative AI for Healthcare Applications
- AI Agent Development for Healthcare Workflow
- EHR & Healthcare System Integration
- HIPAA-Compliant AI Solutions
- Telemedicine & Remote Monitoring AI Systems
- AI Consulting & Strategy for Healthcare
For example, MedTech partnered with a SoluLab team to build a clinical decision support platform that analyzes fragmented patient data integrated with EHR systems.
The solution delivers accurate diagnostics, guideline-based treatment recommendations, and automated clinical documentation, helping clinicians reduce errors and improve patient outcomes.
Book a free consultation call today to get similar results for your business.

Conclusion
Artificial intelligence is no longer an experiment but a necessity in healthcare. The future is not a series of single AI applications, but a collection of integrated, secure, and scalable systems to enhance clinical care, cut spending, and increase access to care.
The difference: Predictive diagnostics to AI-assisted processes and patient monitoring in real-time have an impact that is quantifiable and functional.
But the success in the long run is determined by governance, interoperability, workforce preparedness, and distinct ROI. The strategic investments of healthcare organizations today will help transform the model of care to an elevated, data-driven, and patient-centered care in the coming decade.
SoluLab, an AI development company, can help you build AI platforms or integrate them into existing systems for smoother workflows. Book a free discovery call today!
FAQs
Telehealth AI has the potential to enhance automated triage, symptom assessment, chatbot support, and continuous remote patient monitoring of chronic illnesses, while also expanding capabilities through AI in geonomics for more precise, data-driven healthcare insights.
The primary concerns are data privacy, compliance with the regulations, relationship with the legacy systems, algorithm bias, and high implementation costs. Partnering with AI native companies is the best solution to solve these challenges.
Yes, AI is cost-effective because it automates processes in hospitals, optimizes processes, provides predictive maintenance, early diagnosis, and low readmission rates.
AI examines genetic, lifestyle, and clinical data and applies it to structuring a treatment that is individual to the patient’s profile and thus improves the treatment results.
AI analyzes past and current health data (historical and real-time) to predict the risk of diseases and thus enable early intervention and reduce the total cost of health care.
Neha is a curious content writer with a knack for breaking down complex technologies into meaningful, reader-friendly insights. With experience in blockchain, digital assets, and enterprise tech, she focuses on creating content that informs, connects, and supports strategic decision-making.




